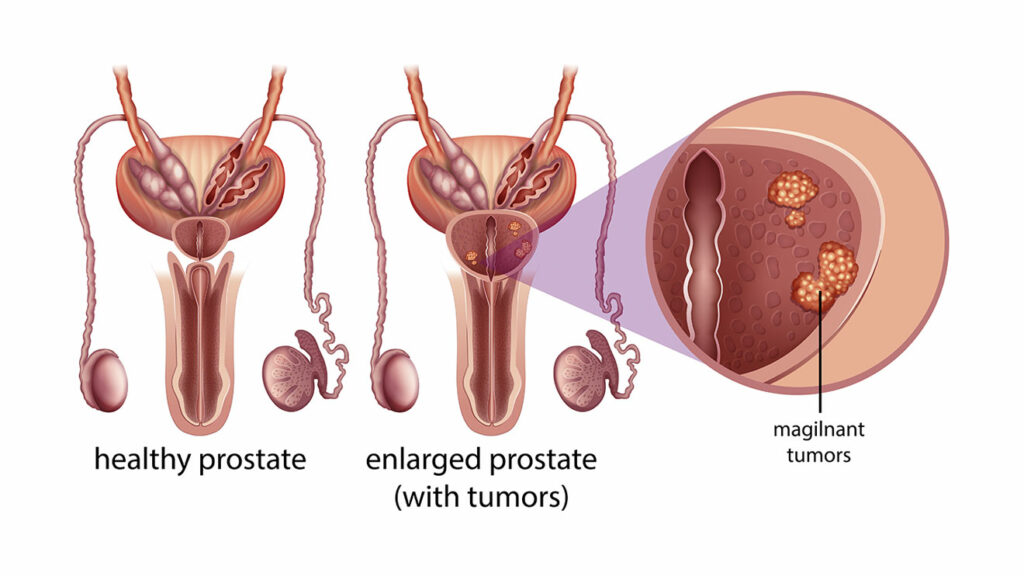
What is prostate cancer?
Prostate cancer occurs when unusual cells form and grow in the prostate gland. However, not all abnormal growths, known as tumors, are cancerous (malignant). On the contrary, some tumors are not cancerous (benign).
Benign growths, like benign prostatic hyperplasia (BPH), are generally not life-threatening.One thing about prostate cancer is that they do not spread to other parts of the body or nearby tissues. Furthermore, you can remove these growths, and though they may grow back slowly, they often do not.
In contrast, cancerous growths, such as prostate cancer, can potentially spread (metastasize) to nearby organs and tissues, such as the bladder or rectum, or even to other parts of your body.
Even if you remove the abnormal growth, there is still a risk of regrowth. In cases where prostate cancer spreads far beyond the prostate, it can become life-threatening, known as metastatic disease.
Is Prostate Cancer Inherited?
Prostate cancer with a family history, known as familial prostate cancer, constitutes approximately 20% of all prostate cancer cases.
This particular form of prostate cancer arises due to a combination of shared genes and shared environmental or lifestyle factors.
Notably, if someone has a first-degree relative, such as a parent, sibling, or child, with prostate cancer, their risk of developing prostate cancer is 2 to 3 times higher than the average risk. This risk escalates even further with the number of relatives diagnosed with prostate cancer.
In contrast, hereditary prostate cancer, which involves inheriting the risk from a relative, is relatively rare, accounting for about 5% of all cases.
Hereditary prostate cancer emerges when genetic changes or mutations are passed within your family from generation to generation, a phenomenon known as autosomal dominant inheritance.
Family history and prostate cancer
You can consider the possibility of hereditary prostate cancer if your family history displays any of the following traits.
- If three or more of your close relatives have had prostate cancer.
- Prostate cancer occurs in three generations of the same family.
- When two or more close relatives, such as a parent, sibling, child, grandparent, uncle or nephew, on the same side of the family are diagnosed with prostate cancer before the age of 55.
At what age is prostate cancer most common?
Prostate cancer is most common in older men. The risk increases significantly after 50, and regular screenings are crucial to detect it at an early, more treatable stage.
Is there a family link to prostate cancer?
Among all the other cancers, it's worth noting that prostate cancer stands out as the most heritable, with genetic factors contributing to approximately 58% of cases.
Looking deeper into the facts about prostate cancer, men may also be at increased risk if any of their family members have had other cancers, such as ovarian, breast cancer, pancreatic cancer or colon cancer.
Since family members share genes, various genetic factors contribute to the risk of developing prostate cancer in the family.
Symptoms of prostate cancer
Prostate cancer may not exhibit noticeable symptoms in its early stages. As it progresses, you might experience symptoms such as
- Difficulty in urination
- Blood in the urine
- Blood in semen
- Difficulty emptying the bladder completely
- Frequent urination during the night.
- Reduced strength of the urine stream
What is the best predictor of prostate cancer?
Prostate-specific antigen (PSA) levels.
Prostate-specific antigen (PSA) levels are a vital indicator of the prostate gland's health.
PSA is a protein produced by the prostate, and it typically remains at low, stable levels in a healthy prostate. Elevated PSA levels can signal various prostate conditions, including prostate cancer and benign conditions like benign prostatic hyperplasia (BPH) or prostatitis.
Physicians often use PSA testing to monitor and assess the prostate's condition, and significant fluctuations in PSA levels can warrant further evaluation to determine the underlying cause.
While high PSA levels can be an early sign of prostate issues, it's important to note that they do not conclusively indicate cancer, you should interpret it in conjunction with other diagnostic tests.
PSA velocity
The level of PSA in the blood can change over time and measuring these changes is a crucial measure to assess the potential risk of prostate cancer.
A significant and rapid increase in PSA levels over a short period may raise concerns and prompt further investigation, as it could indicate a higher risk of prostate cancer.
Gleason score
The Gleason score is a numerical assessment used to evaluate the aggressiveness of prostate cancer based on the appearance of cancer cells under a microscope.
It helps determine the severity of the disease and guides treatment decisions, with higher scores indicating more aggressive cancer.
At what PSA level should one consider a biopsy?
A prostate biopsy can be used to assess the presence of prostate cancer.
Your healthcare provider might suggest a prostate biopsy under the following circumstances: when a blood test reveals an elevated prostate-specific antigen (PSA) level or when an abnormality or lump is detected in your prostate during a rectal examination.
Who should consider getting genetic testing for prostate cancer?
In Sweden, men diagnosed with prostate cancer before 60 years of age and whose cancer has spread outside the prostate and/or with a Gleason score of 5 should be offered genetic testing. In addition, the man has to have a first-degree relative who has been diagnosed with either breast, ovarian, pancreatic, or prostate cancer.
Treatments for Prostate Cancer
Depending on its stage and aggressiveness the treatment options vary. Common treatments include surgery, radiation therapy, hormone therapy, and active surveillance.
Summary
Do not hesitate to proceed in case you qualify for genetic testing for cancer risk, as it helps with treatment decisions and helps your family to be informed about their risks. Undergoing testing can cause concern but has significant benefits for understanding your health risks and making decisions to protect your health.
References
- American Cancer Society What is Prostate Cancer
- National Cancer Institute. Prostate Cancer Treatment
- National Library of Medicine Prostate Cancer

